This is the conclusion of a 4 part essay on the long term effects of wrong sex hormones on men. For Parts I and 2, please see A Man called Hank, Parts I and II. For more detailed information and research, please visit the author’s substack.
Part III: Medicalization
The affirming literature
At first, I looked at the affirming literature that has been covered so glowingly in the press. There are many (and some of them, which have been reviewed here in PITT, are atrociously awful, claiming things that, even with their flawed methodology, they do not show). So I decided to look at the most recent ones that have been published in the most prestigious of journals. For example, take the New England Journal of Medicine – it doesn’t get more prestigious than that. Early in 2023, the NEJM published “Psychosocial Functioning in Transgender Youth after 2 Years of Hormones.”
We should clarify something about this stream of literature straight away. They are primarily concerned about how the patients feel after the administration of hormones or surgery. They are not concerned about the body’s physiological response to these medical interventions. To take an extreme example, if a drug like cocaine was administered to these patients and they then reported feelings of euphoria, this stream of literature would report this euphoria but not consider the other long-term effects of cocaine on the body and the brain
In two wonderfully detailed posts, Jesse Singal goes through the many problems in the paper. For example, the authors started their research project with eight key variables in their study protocol that they submitted as part of their Institutional Review Board (IRB) approval process. However, six of those eight variables – gender dysphoria, trauma symptoms, self-injury, suicidality, body esteem, and quality of life – exactly the type of variables you want to find out in research on mitigating gender dysphoria – are not reported in their published paper. The authors also changed the hypotheses from when they began their research to what they finally presented in their paper.
To put it in more layperson terms, the authors started looking for evidence for something and, upon not finding any of it, tried to pretend that they were looking for something completely different. As Singal points out, this seems to be a textbook case of HARKing, or “hypothesizing after the results are known.” To quote him once again: “...this missing variables issue does call the entire effort into question, simply because if many of the variables the researchers tracked didn’t improve, or even worsened, the fact that they were able to cherry-pick five that did show some improvement might not mean anything at all. We may be looking at nothing but statistical noise – we just can’t say for sure since the researchers are obscuring so many of their results.”
But the authors did find something, right? After all, all medical research is messy, and surely one cannot expect to be 100% certain about every small thing before administering patently “life-saving” care for severely marginalized people who would otherwise commit suicide?
Well, not so fast. As Singal points out in his second post, with the few variables that do improve, the improvements are often so small (and, in one case, not statistically significant either) that the authors themselves classify them as minimal or small (something the paper does not highlight, but can be found in Table S5 in the supplementary appendix: see the “effect size” column). For example, the average depression score goes from “mid” mild (16.4) to “low” mild (14) (scores between 14-19 are considered mild) after two years of hormone treatment. The effect size, 0.20, is at the borderline of insignificant and small. 1
Such “meh” results are nothing new in the field of gender medicine. There have been several studies of truly dubious quality in this area, many of them relying on self-reported surveys (and even there, the data is often so biased that we have no idea about their validity). And yet, prestigious journals continue to publish studies that sometimes even gender affirmists think are too awful.
However, with variables measured by clinicians, especially in longer studies where the subjects were rigorously followed, the psychological results of medicalization have always been “meh.” For example, when it came to puberty blockers, presenting at the WPATH symposium in 2016 in Amsterdam, Polly Carmichael, the Director of the NHS Gender Identity Development Service (GIDS) clinic, reported no changes in psychological functioning or self-harming thoughts or behaviors or gender dysphoric feelings within the clinic’s patients as part of their long-term study that had begun in 2011 to replicate the success of the “Dutch studies.” (In fact, results of the Dutch studies – with all their caveats – have never been replicated anywhere else.)
The elephant in the room in the NEJM study is the alarmingly high rate of suicide among the study subjects, even after the researchers removed the youths with severe psychiatric problems from participating in the study (and the researchers mention that in the study protocol).
Among the 315 relatively stable patients, who on average were only mildly depressed, and were being cared for by “a multidisciplinary team that includes medical and mental health providers,” two committed suicide over the course of the study. In comparison, the Tavistock GIDS clinic in the NHS, the world’s largest pediatric gender clinic (now slated to be closed in 2023), recorded three suicides between 2016 and 2019-20 among its patients or those on waiting lists. This is the clinic where the overwhelming majority of all children and adolescents with gender dysphoria from the entire UK were referred to. Using numbers from the NHS, the annual suicide rate among clinic-referred transgender adolescents in the UK has been estimated at 13 per 100,000. The numbers from the NEJM study? 317 per 100,000 – that’s over 24 times higher.
One cannot claim that the hormones caused the suicides among the patients in the NEJM sample – I’m not an irresponsible researcher, after all – but with these stratospheric numbers, neither can one claim that the hormones helped the youths reduce their suicidal tendencies! However, that did not stop NPR from doing just that. In a recent news report, NPR specifically cited this research to claim that hormones reduced suicidal ideation and attempts. Just how lazy can journalists get? And do they realize how much harm examples like these can do to journalism?
To summarize, therefore: (1) the authors drop six of the eight vitally important variables that they wanted to explore when they began the study, and do not disclose anything about them; (2) they find minimal improvements in a few others, and (3) there is an alarming rate of suicide even among relatively stable youths who are cared for in some of the top clinics in the country. These results – milquetoast at best and extremely alarming at worst – did not stop the researchers from claiming that there is “robust scientific evidence” for hormone treatment for better mental health outcomes among transgender and nonbinary youth.
At this point, let us pause and note that there is no control group in this study. Advocates for affirmation would have us believe that these medications are so life-saving that preventing the kids from having access to medicalization within a study would be cruel. However, after looking at the alarming rate of suicide (even among the more stable patients, who were regularly looked after in some of the top hospitals in the country), with many critical variables not reported, and with minimal improvements in the remaining variables, one has to ask the question – why not have a control group? What if – as was argued in the Archives of Sexual Behavior in November 2022 – all we are seeing is a perfect storm of placebo (and nocebo) effects, and we have no idea at all as to what happened? (Well, actually, we do, but more of that later.)
I digress. I started to find out what can be expected from the medical interventions for young AMAB (assigned-male-at-birth) trans women like my son. And there, the researchers of the NEJM study are unequivocal about their findings: even among the variables that were finally reported, “depression and anxiety scores decreased…but not among those designated male at birth.”
Screenshot from page 5 of the NEJM study
That’s right. For young men like our son, even those researchers who believe in “full steam ahead with hormones” have nothing optimistic to report. Zip. Nada.
Looking back, that shouldn’t have been much of a surprise to the researchers. After all, they would have been aware of the study (with its famous lead author) that had come out exactly a year back in PLOS One, where the authors claimed that access to hormones during adolescence led to “better mental health outcomes” among transgender adults. However, by dissecting the same data (i.e., the 2015 U.S. Transgender Survey), it was shown that estrogen is associated with nearly double the rate of suicidality for young men. 2
These findings on the psychosocial effects of estrogen on natal males, in turn, replicate what was found from a larger (and longer-lasting) study conducted across three gender clinics in Belgium, Italy, and the Netherlands and published in 2021. Following 873 patients undergoing hormone treatment over three years, researchers found very little change in their mental outlook (if anything, the scores were almost uniformly lower for trans women all along).
But so much for patient surveys on their mental outlook and how they feel. How does the body react physiologically to estrogen? To go back to the cocaine analogy I introduced earlier, we do not willy-nilly administer cocaine to patients just because they feel some initial euphoria (which, in the case of estrogen, is ironically conspicuous by its absence). What do the clinical studies on the effect of estrogen on the brain and the body say
Estrogen and the male brain
While not explicitly focused on transgender issues, the research in the last few years in the areas of endocrinology, neuroendocrinology, and neuroscience have given us a much better understanding of the effect of hormones on the brain. Neuroendocrinology used to be the branch of medicine investigating how the brain controls the endocrine system via the hypothalamus and pituitary gland. It has now evolved into a branch that includes studying how hormones affect many aspects of brain function. Research in this area – much of it occurring in the past decade – has changed the way we think of the effect of estrogen on the male brain.
In 2018, researchers from Germany showed that increased estrogen levels are associated with depression in males. No wonder all the patient survey studies, including the latest in the New England Journal of Medicine, showed no improvement in the psychological outlook among males.
Psychoneuroendocrinology, Volume 87, January 2018
Two years later, in 2020, researchers from Spain discovered why estrogen might act this way by administering pharmacological doses of estradiol in adult male rats. They found that when treated with estrogen, the brains of adult male rats show changes similar to those observed in the brains of trans women. As a result, they could now thoroughly examine what these changes were. (As always, we humans have the rodents to thank for many of our medical advances. Thank you, mighty mouse!)
Highlights from the paper in Hormones and Behavior, Volume 125, September 2020
What are these changes? The authors highlighted them at the beginning of the article. One of the effects of estrogen is to reduce the water content within the glial or “glue” cells called astrocytes and the oligodendrocytes (more on that a bit later) as well as the axons in the brain, thereby reducing the cortical white matter integrity in the brain. This is important because reduced white matter integrity is related to cognitive instability.
By reducing the water content, the estradiol increased the relative concentration of glutamate and glutamine in the brain, an excess of which, as the Cleveland Clinic notes, is associated with such diseases as Parkinson’s, Alzheimer’s, and Huntington’s disease.
Estradiol also decreased the brain cortical volume, which has been shown to be positively associated with general intelligence (in other words, a decreased cortical volume will generally predict a lower level of general intelligence). Recent neuroimaging studies (in 2020) have linked lower cortical volume and thickness in patients with schizophrenia and bipolar disorder.
Evidence from the real world backs up these findings. In 2020, researchers from the Alzheimer's Disease Research Center at the University of Wisconsin School of Medicine and Public Health presented their findings that showed a 37% higher prevalence of subjective cognitive decline, which is an early sign of Alzheimer’s disease, among transgender and gender nonbinary adults in the US.
Let’s go back to those glial cells. In the past few years, there has been a wealth of research on these cells in our brains, and this research indicates that these cells do much more than merely being the “glue” that binds everything in the brain.
“Neurons are not the only brain cells that think,” The Economist, January 23, 2023
We now know that misbehaving glial cells are the culprit behind a range of conditions, from autism to multiple sclerosis to obsessive-compulsive disorder. Astrocytes play a crucial role in memory formation, consolidating relevant short-term memories into long-term ones (I got reminded of the “brain fog” that Hank mentioned he suffers from, as well as what the parents said about their male children who had suddenly become less capable mentally after starting hormone therapy). Disorders in astrocytes are related to a wide range of different neuropathologies. There is evidence that malfunctioning astrocytes contribute to mental illnesses like schizophrenia, mood disorders such as depression and anxiety, drug dependence, mental retardation, and neurodegenerative diseases like Alzheimer’s.
Interestingly, it has been shown that the brains of depressed suicide victims had a markedly lesser volume of astrocytes than healthy brains. So, when estrogen reduces brain cortical volume and increases the relative concentration of glutamate and glutamine, not only do many neuropathologies follow, but the subjects also become depressed and more liable to commit suicide. This is not an overnight process but more akin to a slow-moving train wreck that reaches its climax over the next several decades. Transgender activists would have us believe that suicide among transgender people stems from their marginalization. That is definitely a possibility. However, the research from the past few years provides a more “Occam’s Razor” explanation: after the estrogen treatment, their brains gradually become more susceptible to committing suicide.
In this context, it is interesting to note that among two other marginalized groups – gay men and black men – suicide is not a leading cause of death. Gay men do show higher risks of mortality than strictly heterosexual men; however, that increased risk comes only from HIV: “mortality risk from non–HIV-related causes, including suicide, was not elevated [emphasis mine] among MSM [men who have sex with men].” And, among black males, as a percentage of all deaths, suicide does not figure among the ten leading causes of death. However, it does among non-Hispanic white males. Suicide is one of the leading causes of death among younger black males, but even there, it is significantly more pronounced among younger white males. So, their marginalization does not lead gay or black men to commit suicide – at least when compared to their peers.
Estrogen and cardiovascular system
The hormones have other effects too on the rest of the body. For example, a large-scale study from 2018 among transgender patients in the US showed that, compared to men, the incidence of venous thromboembolism or VTE (or blood clots, which include deep vein thrombosis and pulmonary embolism) among trans women is 50% higher within the first two years of hormone treatment and more than five times higher in follow-ups beyond two years. The incidence of ischemic stroke (when the blood supply to part of the brain is interrupted or reduced, resulting in the brain cells dying within minutes) is 30% higher within the first two years and nearly ten times higher in follow-ups beyond two years. The authors conclude that "[t]hese results… indicate the need for long-term vigilance in identifying vascular side effects of cross-sex estrogen." These results weren’t outliers either – they were replicated by researchers at the Amsterdam clinic in 2019.
Estrogen and the immune system
Adult women are disproportionately more prone to allergies, asthma, and autoimmune diseases than men (growing up, boys have more allergies than girls, but the ratios flip completely after puberty), but the huge spike of synthetic estrogen hormones changes that equation for trans women. For example, one parent I talked to mentioned how their son used to love cats and be the prime caretaker of the family’s cats and is now (after hormones) completely allergic to them. Estrogen skews the body’s immune responses toward allergy and worsens asthma attacks, and its deleterious effects gradually progress to more severe autoimmune diseases.
There are case studies of increased immune-mediated rheumatic diseases (IMRD) such as rheumatoid arthritis (Hank mentioned this as one of the things he suffers from), spondyloarthritis (characterized by low back pain – another of Hank’s ailments), systemic lupus erythematosus (the most common type of lupus, where the body’s immune system attacks its tissues in joints, skin, brain, lungs, kidneys, and blood vessels), systemic sclerosis (this is the same as the scleroderma that Hank mentioned), and vasculitis (where blood vessels – both arteries and veins – are destroyed), as well as the onset of other autoimmune diseases among trans women.
One parent I met recently mentioned how their son suddenly developed Crohn’s disease after starting hormone therapy – already, his daily regimen is up to 8 medications. A 31-year-old male detransitioner mentions developing scoliosis and osteoporosis after hormone therapy, both of which, while not autoimmune diseases themselves, are linked to – as outcomes of – autoimmune diseases.
Our understanding of these diseases (76 of them, by the last count), when the immune systems that are supposed to defend our bodies from diseases but attack us instead, is still evolving. Many of them have no known cure. However, we now know that nearly 80% of the autoimmune sufferers are female, and it is now clear that, with some exceptions, many autoimmune diseases “are driven by estrogen,” specifically by spikes of estrogen in the body. For example, Scientific American noted that “oral contraceptives and hormone-replacement therapy, both of which add estrogen to the body, has been linked to an increased risk for lupus.”
Research has also shown a “strong association” between gender identity disorder and multiple sclerosis in transwomen, indicating “a potential role for low testosterone and/or feminizing hormones on MS risk” among natal males.
Estrogen also decreases insulin sensitivity (also known as increasing insulin resistance among diabetes patients) in trans women, which is a sign that the body is having difficulty metabolizing glucose, and this can indicate wider health problems such as high blood pressure and cholesterol levels.
Each one of the ailments that Hank told me he suffers from appears in these case studies. While our son will never have all the characteristics of a woman, he will nonetheless experience womanhood through its diseases. With so many new diseases to choose from! Add to this list the possibility of retinal detachment that Hank and several of his male-to-female transgender acquaintances suffer from.
We should remind ourselves that the recent research probably vastly undercounts both the incidence of disease and the diseases themselves. Historically, the medical establishment could be least bothered by what was happening to an impoverished, marginalized population that stayed in the shadows and was considered freaks by the general public. There was no money there. When they died, nobody cared, and there was no autopsy or investigation. Any “research” carried out was by a few “doctors” who handed out off-label drugs or performed surgeries away from the spotlight. If these doctors came to know or suspect anything, they had no incentive to publicize those findings to the general public and “out” themselves and kill those revenue streams. There were no gullible journals or conferences to virtue-signal their junk research in. All the while, these people died an early death. And those early deaths are staggering.
Rheumatoid arthritis, Systemic sclerosis, Vasculitis, and Chronic Discoid Lupus Erythematosus
Estrogen and the incidence of cancer among men
Other than the risk of hepatocellular carcinoma or liver cancer that I alluded to earlier, an “ample body of evidence” suggests that “estrogens may play a critical role in predisposing, or even causing, prostate cancer.”
And in 2015, publishing in the Journal of Clinical Oncology, researchers found that “circulating estradiol levels showed a significant association” with the occurrence of breast cancer among men.
I guess we have to be thankful. At least these men do not have ovaries and uteruses. Because women have to deal with those types of cancers – and once again, estrogen is to blame.
Estrogen and the liver
And while we are dumping on poor estrogen, let us also note that higher doses of estrogen have been associated with several liver-related complications, including “intrahepatic cholestasis, sinusoidal dilatation, peliosis hepatis, hepatic adenomas, hepatocellular carcinoma, hepatic venous thrombosis and an increased risk of gallbladder stones.” Remember Hank’s gallbladder stones? While these ailments were more commonly seen with higher doses of estrogen, they have also been described with low-dose estrogen hormone replacement therapy.
Mortality after hormones
Depression, mental disorders, cardiovascular diseases, autoimmune diseases, and increased suicidal thoughts – it is perhaps no wonder the overall mortality risks of transgender women are so much higher than the general population (this landmark study looked at the mortality risks of transgender people in the Netherlands over five decades, between 1972 and 2018). The deaths were attributed to cardiovascular disease (21%), cancer (32%), HIV-related disease (5%), and suicide (7.5%). Significantly, even though the risks of dying from HIV have decreased over the past few decades (and also, presumably, the stigma against transgender people is lower now than it was fifty years back), the mortality risks did not reduce over time. Once again, these results have been replicated among US transgender patients by researchers at the University of Michigan and Brown University in their research that was published in 2022.
At this point, it is so surreal to see that it is parents like us, coming from fields far removed from biology and medicine, who are taking all their time from their day jobs to go through this research. For many, it has affected our professional and personal lives, not to mention our physical health and well-being.
As for the people who should have been doing this job and acting as gatekeepers – the psychologists, the endocrinologists, the doctors and the nurses, and the entire medical profession – why, they all have resorted to magical thinking and activism and even claiming that “although gender-affirming hormones can cause some irreversible changes,…these effects are primarily cosmetic.”
Shrinking brains, cognitive decline, depression, Alzheimer’s, suicide, cardiovascular diseases, asthma, arthritis, systemic sclerosis, Crohn’s disease, lupus, and other autoimmune diseases – yes, according to the gender “experts,” all these changes from estrogen are “primarily cosmetic!”
Do these people truly not know or understand the research, or are they intentionally misleading the general public? At this point, I don’t know which is worse – a scientific inquiry led by idiots or truly reprehensible human beings. Does the American medical establishment realize how much harm it is doing to its long-term reputation by allowing such idiots and/or charlatans to lead this diabolical charade? And all this for what? Some lazy likes on their Twitter feed? Some feeling of easy virtue? A bit of filthy lucre?
However, we do know one thing: the previous generation of the medical establishment could hide behind “we don’t know,” but that no longer applies to the current generation of doctors and psychologists, especially after we have held the research in front of them.
After Surgery
So, the hormones won’t help my son – psychologically or physically. Rather, they will hasten his cognitive decline and increase his risk of getting into depression. It will also significantly increase his risk for cardiovascular diseases and autoimmune diseases. All of which will drive him to suicide if he hasn’t succumbed to them already. All these developments might nudge him towards surgery, after which he might hope to pass better as a woman.
Unfortunately, the mortality rates are even worse after surgery than they are after hormones – which is ironic since, if the activists are to be believed, the surgeries should have led to a more fulfilling life for a transgender woman in their quest to become their “authentic” self.
One reason behind these deaths? The postoperative complications, which are widespread, right from the very beginning.
In early 2023, researchers unveiled the results from Canada's first vaginoplasty postoperative care clinic. Nearly a quarter of the trans women who were operated on accessed follow-up care in the first three after surgery, and more than half sought care within the first year. More than three-fifths (61.3%) were seen for more than one visit and presented with more than two symptoms or concerns.
The most common patient-reported symptoms during clinical visits included pain (53.8%), dilation concerns (46.3%) (this is because the body, apparently not getting the memo from the mind, identifies the neovagina as a gaping wound, and so it has to be dilated for life, including multiple times daily during the first year: the aftercare regimen from the clinic runs into eight pages!), and surgical site/vaginal bleeding (42.5%). Sexual function concerns were also common (33.8%), with anorgasmia (inability to orgasm) (11.3%) and dyspareunia (painful intercourse) (11.3%) being the most frequent complications. The most common adverse outcomes identified by healthcare providers included hypergranulation (38.8%), urinary dysfunction (18.8%), and wound healing issues (12.5%).
We aren’t done yet. A review of the literature from 2018 on complications of the neovagina in trans women after surgery shows an overall complication rate of 32.5% (i.e., about one in three cases) and a reoperation rate of 21.7% (more than one in five cases) for “non-aesthetic reasons.” Another paper (also from 2018) discusses various neovaginal complications in transwomen: stricture of the neo-urethra, leading to urinary tract infections; scar tissues in the neovagina, causing it to become narrower and shorter; “intravaginal hairballs;” vaginal prolapse (when the top of the vagina weakens and collapses into the vaginal canal) and recto-vaginal fistulas (a tunnel between the vagina and rectum, leading to rectal discharge through the vagina, which could occur even during sex).
It is difficult for anyone to come to terms with these setbacks – especially if they had been promised a life of fulfillment afterward. But those who do talk mention that their life has been a “living hell since then.” Another detransitioner asserts, “This is not rare.”
Many of these complications will remain with the patients for life, affecting their basic day-to-day activities from morning till night (one such account makes for harrowing reading: “managing the trickle of urine from my constricted urethra after going to the toilet, the occasional shooting pain and the despair of my own stupidity”). Is it a surprise if many succumb to these complications – or commit suicide – so early in their lives?
Let’s take a minute now to list what my wife and I can expect to happen with our son (and since the research is ongoing, this is probably an incomplete list):
After hormones, there’ll be no change in his psychosocial well-being. There’ll be no change in the overall quality of his life.
However, if anything, he will be at a higher risk of suicide.
His brain will gradually shrink, leading to depression, and…
…over the longer term, he will see the gradual incidence of cognitive decline and neuropathologies like early-onset Alzheimer’s, schizophrenia, loss of memory, and other disorders.
He will develop new allergies and possibly asthma. He will become prone to many autoimmune diseases, like rheumatoid arthritis, systemic sclerosis, vasculitis, and lupus. His immune system will attack his joints, skin, brain, lungs, kidneys, and blood vessels.
He will be at a heightened risk of cardiovascular diseases, especially after the first couple of years, leading to lifelong medication – and possible heart attacks and emergency visits all his life.
If he later opts for an orchiectomy, his sex drive will completely cease, and he won’t have any sexual intimacy for the rest of his life.
If he further opts for vaginoplasty, he will have to make repeated and regular visits to the surgery room for many different complications – even for basic functions like urinating, let alone urinary tract infections or recto-vaginal fistulas – for the rest of his life. (And since he is in the US, let’s hope he will have a sympathetic employer to let him keep his job and health insurance despite his many absences. As NPR discovered, the first-time costs can run into six figures, never mind the cost of the lifelong follow-up visits.)
And finally, what with all the physical ailments, mental diseases, and the decrease of his mental faculties starting from a very early age, he will have a much higher risk of early death from one or more of these conditions – or he might decide to end it all by committing suicide.
With all these “benefits” of medicalization, who needs to research any pesky problems? But then again, what do I understand about my own son’s health and happiness?
The WPATH Standards of Care Guidelines 8 document states in its abstract that its aim is “...to assist TGD [transgender and gender diverse] people…optimizing their overall physical health, psychological well-being, and self-fulfillment.”
What kind of “physical health, psychological well-being, and self-fulfillment” will our son – or, for that matter, any trans woman – get from hormones and surgery? Is it the superior physical health that comes from shrunken brains and blood clots in the brain, and heart attacks? Or maybe the psychological well-being comes from early Alzheimer’s and schizophrenia, and depression? Or the feeling of self-fulfillment that comes from ending life early from suicide?
So many of Hank’s friends did not have to choose – they got all three.
Part IV – What to expect over the years
I realize the bitter irony in this for my wife and me. As the dangers of medical transitioning become increasingly understood, there is a feeling that “peak trans” is probably over. Mainstream media seem to have caught on to the madness. Professional bodies like the British Medical Association are increasingly direct in stating what we parents have suspected for a while – that GAC (i.e., gender-affirming care) is not evidence-based. The explosive Jamie Reed whistleblower account reiterated a similar madness when she exposed what was happening in The Washington University Transgender Center at St. Louis Children's Hospital (and then Jesse Singal bared the dishonesty of those involved in trying to bring her down). That should put other centers under greater scrutiny as more people see Reed’s brave example to emulate.
The searing account of what happened in the GIDS clinic in Tavistock, the world’s largest pediatric gender clinic (until its announced closure in 2023), a place whose doctors most commonly described as “mad,” is another important pitstop on the road to sanity. Do consider reading the book: you will read what happened in the UK in the 2010s, where the NHS Gender Identity Development Service, under pressure from activist organizations like Mermaids (now under investigation) and under severe strain from the rapid influx of a new generation of adolescent patients who identified themselves with gender dysphoria, gave up their prevalent model of care – one that emphasized extended psychological counseling – in favor of rapid medicalization. Fortunately for the British, sanity seems to be on its way.
Unfortunately, all this good news might come too late to save our son. It isn’t easy to escape the claws of the online activists and narcissists and the “trans-tech” industry that estimates the average transition cost at $150,000 per person. And most tragically, he transitioned after 18—as an “adult.”
In her blog, the ever-thoughtful and recently detransitioned woman, Michelle Alleva, pointed out that in the coming years, those who transitioned as young adults – however vulnerable and misinformed they might have been – will not find any sympathy or support. Young children who medically transitioned before 18 might be seen as innocent victims. However, those who transitioned after 18 – never mind that they were barely adults, with their still-developing brains far from full maturity – will be merely seen as just one more of the mentally ill. As someone recently commented on Twitter, “If you're 18 and think you're the opposite sex, you have a mental illness. If you're 8 and think you're the opposite sex, your mother has a mental illness.”
In the coming years, there will be many people who, back in the day, identified as transgender or non-binary or anything in between and will be reminded of their youth as they look at my son and tell their children, “Thank heavens I stopped before making that mistake!” and beat a hasty retreat from his presence. Our son will be the cautionary tale.
My wife and I stay awake every night, thinking about what will happen to him. Years later, even as he realizes that the medical experiments on him have been a series of colossal mistakes, it will get increasingly difficult to admit that. Especially to an uncaring world that has long moved on. What else will he have left to cling to? Can you imagine how it feels to realize that everything you were told was lies and there is no way to turn back the clock? That all those “brave” statements you made are now seen as hollow remarks made by a callous young person without mental maturity? With all the public outpouring of scorn directed towards him, it would be “really easy to slip into the mindset that everyone hates me, I’m a medical monster, I’m bad and evil, and I deserve this.”
All of us have made our share of stupid statements in our youth. That’s one of the rites of passage to adulthood. But then we are afforded the benefit of time to paper over our youthful misadventures. That is a luxury that will be denied to our child. Every new disease he inherits from this cult, every latest visit to the emergency, and every recoil from people he encounters on the street will remind him of what he has wrought upon himself.
It took Hank forty years to come to grips with his mistakes.
But still, Hank is lucky. Even though, by his admission, he has trouble remembering things and suffers from brain fog, he still retains some of his mental faculties, unlike some of his friends. Unlike some of his other friends, he is still alive to tell the tale at 70… after the kidney stones, the gallbladder stones, the liver stones, the saliva channel stones, the heart attack, the hypertension, the arthritis and the back pain, the asthma and the allergies, the scleroderma, the retinal detachments, the lifelong visits to the VA, and the fistful of medications every day. He has finally managed to look at himself and accept what he saw. His friends, unfortunately, didn’t have that chance.
Hank is also fortunate that he has the VA healthcare system to take care of him when he lands up there with his latest medical episode. Our son won’t have that. Will the doctors and the nurses and the psychologists who are telling our son today that hormones are safe, or the researchers who claim that these medical interventions are “primarily cosmetic,” be there for him to hold his hand and pay his bills when he goes to one clinic after another with his various ailments…with his schizophrenia and depression and anxiety and drug dependence and possibly several neurodegenerative diseases? With his blood clots and his autoimmune diseases? Or when he is in an emergency room because of his latest suicide attempt?
Or will it be left just us – my wife and I, these two old transphobes – like Hank’s (or D’s) hapless mother, trying to find a way to help their adult man-child whom the society has chewed, spat out, and completely forgotten?
The only large effect of the hormones that the authors find is in “appearance congruence” – which, come to think of it, is the least that can be expected from the hormones. I mean, if the hormones had failed to deliver even on making one’s appearance becoming more congruent to the gender they identify with, what would they have achieved?
Not only that, their data showed that puberty suppression is not associated with better mental health outcomes for either sex. Another comment pointed out that the same data shows that access to the hormones was correlated with increased past-year suicide attempts

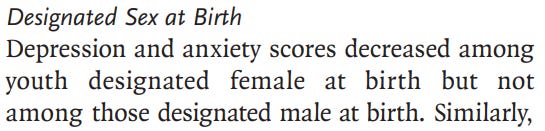




This is a very moving, informative, and thought-provoking set of essays. I thank you very much for taking the time, the effort, and the heartache to share your thoughts and your journey. Believe me, if there were anything I could do to make this mess go away, I would. Unfortunately, I think you're correct in that it will take a long time for everyone to return to reason, if, in fact, they ever do.
Your rhetorical question as to whether the medical establishment knows what harms come from cross-hormone treatment can be answered quite simply, "Yes they do." People in the biomedical field have known this for over half a century, at least. I wrote about this irony in a Substack essay about cross-hormone (androgen) administration to female Olympic athletes, and referenced what we know about therapeutic hormone suppression for male cancer patients, as have others. Likewise, you have cited a number of studies including animal model studies that provide additional evidence as to the problems and effects of hormone suppression and administration. None of this is that difficult to understand. However, what is difficult to understand — and what I try to teach in virtually all my physiology lectures — is the intricate complexity of all physiological and neural systems. Unfortunately, many people (including many of my pre-med students, and practicing physicians) don't appreciate that point. Many see physiology as a series of switches that can be turned on and off, and a series of parts that can be swapped out at will. However, biology doesn't work like that. Physiological systems (including neural systems) are complex, highly integrated, multi-determined, and non-ergodic. In short, if you mess around with one part, it's going to have broad, profound, and often unexpected consequences system-wide. That's inevitable. You made that point very well in your essays. And, please understand that I'm very sincere in saying that many physicians, and virtually all of the popular science writers and journalists that I read do not understand the complexity of these systems. (I tried to make that point here: https://everythingisbiology.substack.com/p/there-is-biological-evidence-for) . On the other hand, researchers generally do understand the complexities. Unfortunately, however, they are not the ones making policy or doing the surgery-for-profit.
As you made clear, it is well recognized — or should be well-recognized — that you cannot change an organism into something else via cosmetic surgery and hormone manipulation. As a scientist (and psychologist), I am absolutely astounded by what's happening in this arena. And, my heart aches for the inadvertent, uninformed victims of this ideology and their families.
I wish the very best for you and your family. Thank you again for bringing your thoughts and so much valuable information to the community. Sincerely, Frederick
A note about the most prestigious medical journals - you cannot believe the majority of what they publish anymore. They have been totally captured by the pharmaceutical companies and have been politicized. A long-time editor of The New England Journal of Medicine, Marcia Angell, MD, resigned over this very issue. This is one of her quotes: "It is simply no longer possible to believe much of the clinical research that is published, or to rely on the judgment of trusted physicians or authoritative medical guidelines. I take no pleasure in this conclusion, which I reached slowly and reluctantly over my two decades as an editor of The New England Journal of Medicine."
There is so much to be said and detailed out about this issue there wouldn't be enough space in a comment section.